
“This study demonstrates one of the highest diagnostic yields, by strict definitions, since the development of robotic-assisted bronchoscopy”
- Dr. Amit "Bobby" Mahajan
Mahajan AK, Duong DK, Cortes J, Bhadra K. The match 2 study: Robotic assisted bronchoscopy with integrated imaging with assessment of digital tomosynthesis (DT) and augmented fluoroscopy (AF): Three-Dimensional accuracy as confirmed by cone beam computed tomography (CBCT). Respir Med. 2026 Mar;253:108693. doi: 10.1016/j.rmed.2026.108693. Epub 2026 Jan 29. PMID: 41620189.
Purpose: Navigational bronchoscopy has long faced challenges in reliably accessing and sampling small peripheral pulmonary nodules. The Galaxy System is a robotic-assisted image bronchoscopy platform that integrates digital tomography (DT) and augmented fluoroscopy (AF) for real-time lesion localization. This study examines Galaxy System’s DT algorithm and AF performance. We assessed tool-in-lesion (TIL) and center strike (CS) rates using cone beam computed tomography.
Methods: This prospective two-center study was conducted between November 2024 and August 2025. Thirty-one patients with peripheral pulmonary nodules underwent robotic bronchoscopy with the Galaxy System, performed by three bronchoscopists. Navigation was guided by DT and AF. To assess accuracy, a tool (needle) was optimally placed within the lesion. Cone-beam CT (CBCT) was subsequently performed to verify needle position. Collected data included tool-in-lesion (TIL) confirmation, and diagnostic yield based on definitive histopathology.
Results: The cohort included 16 females and 15 males, with a mean age of 65 years. In total, 31 lung nodules were successfully biopsied. The mean lung nodule size was 16.99 mm (± 6.2 mm) Approximately one-third of nodules were pleural-based, and a bronchus sign was present in only 13% of the target nodule. The mean procedure time was 46 minutes and the average radiation dose from TiLT+™ sweeps was 59.1 mGy. Procedural success, defined as successful deployment of the biopsy tool within the lesion using the Galaxy System, was achieved in all cases (100%). TiLT+ tomography demonstrated tool-in-lesion (TIL) in 30 of 31 nodules (97%), with one case showing tangential tool-touch-lesion (TTL) contact. Of the 30 nodules with TIL demonstrated by a TiLT+ sweep, CBCT subsequently confirmed TIL in 29 (concordance rate 96.7%), with 17 demonstrating center-strike localization (54%). Using strict definitions, overall diagnostic yield was 96.7%, consisting of 20 specific malignant and 10 specific benign diagnoses. Pneumothorax occurred in 1 of 31 cases (3%).
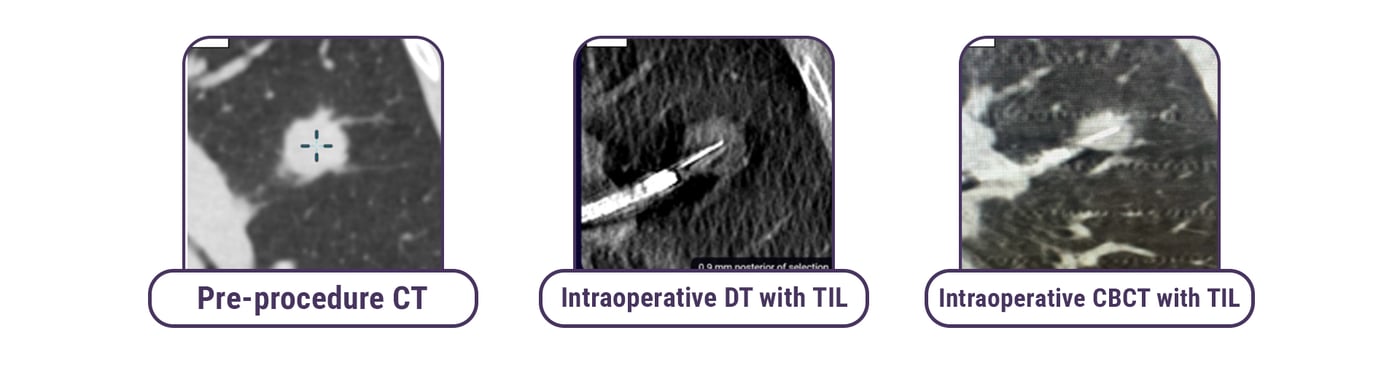

Conclusions: The Galaxy System with Digital Tomosynthesis (DT) and Augmented Fluoroscopy (AF) demonstrates a high Tool-in-Lesion (TIL) and diagnostic yield. The strong concordance between a TiLT+ sweep and CBCT confirmation suggests the reliability of TiLT+ technology for real-time intraprocedural guidance.
